Meningitis
Meningitis is an inflammation of the meninges, the membranes covering the brain and spinal cord. It is a devastating disease and remains a major public health challenge. The disease can be caused by many different pathogens, but the highest global burden is seen with bacterial meningitis, which is estimated to case more deaths in children under 5 years of age than malaria.
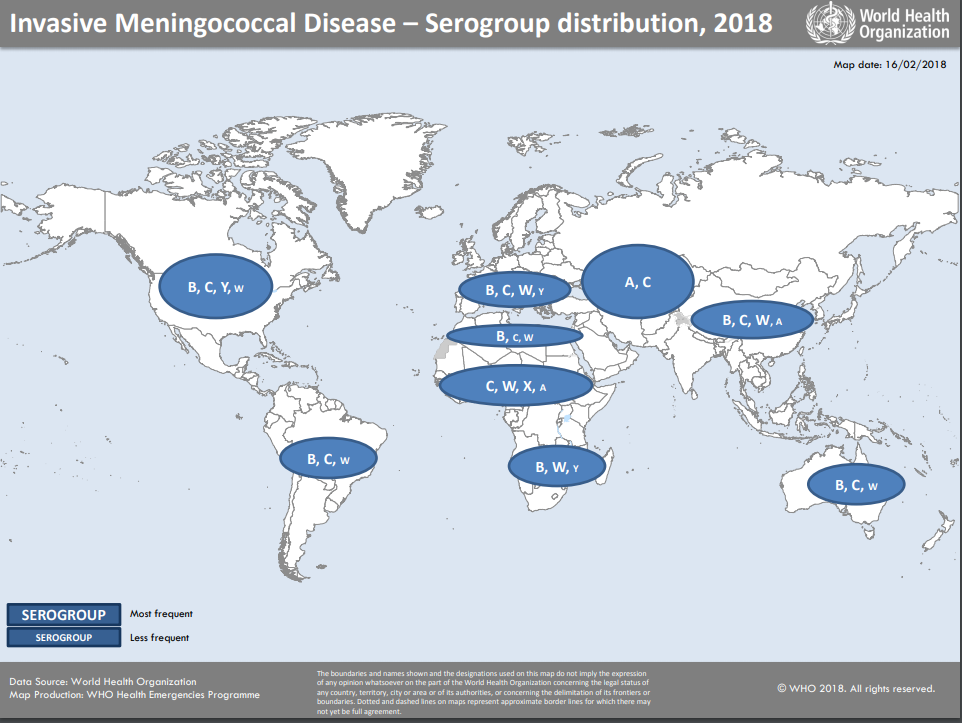
Several different bacteria can cause meningitis. Neisseria meningitidis is the one with the potential to cause large epidemics. Geographic distribution and epidemic potential differ according to serogroup.
Transmission
The bacteria that cause meningitis are transmitted from person-to-person through droplets of respiratory or throat secretions from carriers. Close and prolonged contact – such as kissing, sneezing or coughing on someone, or living in close quarters with an infected person, facilitates the spread of the disease. The average incubation period is 4 days but can range between 2 and 10 days.
Neisseria meningitidis only infects humans. The bacteria can be carried in the throat and can sometimes overwhelm the body's defences allowing infection to spread through the bloodstream to the brain. It is believed that 10% to 20% of the population carries Neisseria meningitidis in their throat at any given time.
The most common symptoms of meningitis are a stiff neck, high fever, sensitivity to light, confusion, headaches and vomiting. Even with early diagnosis and adequate treatment, 5% to 10% of patients die, typically within 24 to 48 hours after the onset of symptoms. Bacterial meningitis may result in brain damage, hearing loss or a learning disability in 10% to 20% of survivors. A less common, but even more severe (and often fatal), form of meningococcal disease is meningococcal septicaemia, which is characterized by a haemorrhagic rash and rapid circulatory collapse.
Diagnosis
Initial diagnosis of meningococcal meningitis can be made by clinical examination followed by a lumbar puncture showing a purulent (contains pus) spinal fluid. The bacteria can sometimes be seen via microscopic examination of the spinal fluid and diagnosis is supported or confirmed via laboratory diagnosis.
Laboratory materials for the diagnosis of bacterial meningitis by PCR
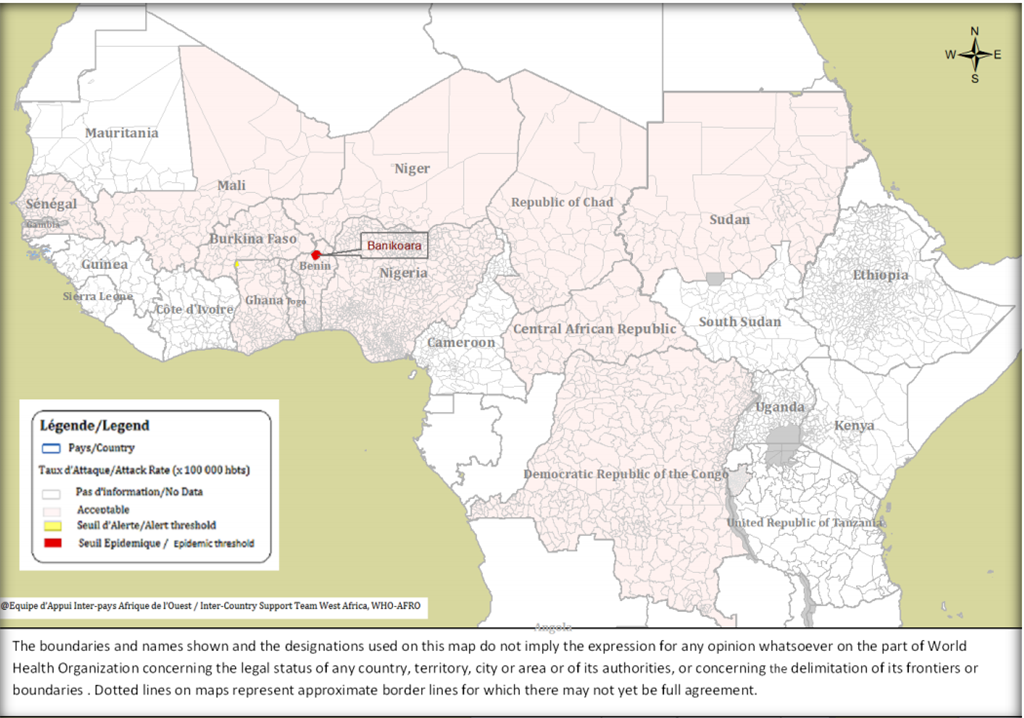
Rapid diagnosis is essential, not only for individual patient management, but also for managing epidemics, particularly in the African meningitis belt. The development and promotion of heat-stable rapid diagnostic tests which detect a range of common bacterial-causing pathogens has been recommended as a priority by a group of WHO-convened experts.
Meningitis diagnostic use cases
Meningitis rapid diagnostic test target product profile
Developing a new generation RDTs for meningitis
Meeting report, 9 March 2018
Treatment
Meningococcal disease is potentially fatal and is a medical emergency. Admission to a hospital or health centre is necessary and appropriate antibiotic treatment must be started as soon as possible.Vaccines and immunization
Licensed vaccines against meningococcal disease have been available for more than 40 years. Over time, there have been major improvements in strain coverage and vaccine availability, but to-date, no universal vaccine against meningococcal disease exists. Vaccines are serogroup specific and the protection they confer is of varying duration, dependent on which type is used.
Since 2010, a meningococcal A conjugate vaccine has been rolled out through mass preventive immunization campaigns in the meningitis belt of sub-Saharan Africa, dramatically bringing down cases of the A serogroup.
There are three types of meningococcal vaccines available:
- Polysaccharide vaccines used in outbreak response, mainly in Africa
- Conjugate vaccines used in prevention and outbreak response.
- Protein based vaccine, against N. meningitidis B. It has been introduced into the routine immunization schedule (one country as of 2017) and used in outbreak response.
International Coordinating Group (ICG) on vaccine provision for meningitis
The Meningitis Vaccine Project - frequently asked questions
Prioritization tool for Meningitis A Conjugate Vaccine Introduction
Chemoprophylaxis
Giving antibiotics promptly to close contacts of anyone infected with meningitis, can decrease the risk of transmission
Surveillance
Surveillance, from case detection to investigation and laboratory confirmation, is essential for the control of meningococcal meningitis in order to ;detect and confirm outbreaks; monitor trends,; estimate disease burden and the antibiotic resistance profile; monitor specific meningococcal strains; and estimate the impact of meningitis control strategies, particularly preventive vaccination programmes.